The WATCHMAN device is a groundbreaking implant offered at PeaceHealth St. Joseph Medical Center. It’s only been available locally since 2017 and is truly changing the lives of patients with atrial fibrillation in a myriad of ways.
Dr. John MacGregor, associate medical director of cardiac electrophysiology with PeaceHealth St. Joseph, has personal reasons for appreciating the WATCHMAN procedure.
“When I was in med school, my maternal grandfather needed a blood thinner for atrial fibrillation, and every time they put him on Coumadin (blood thinner medication), he would bleed somewhere from his gut,” he recalls. “The doctors would have to stop coumadin to address the bleeding. Then they would put him back on it, and he would eventually bleed again.”
At the time, Coumadin was the only oral blood thinner available, and Dr. MacGregor’s grandfather was forced to take a medication that had terrible side effects for him.
“He eventually had a massive stroke when he was off Coumadin, and wound up in a nursing home, unable to speak and care for himself. He existed like that for a few weeks, and then he died,” says Dr. MacGregor. “As a medical student at the time, I thought it was tragic, and I wished we had something else to offer him.”
Dr. MacGregor kept an eye on the WATCHMAN procedure from the research stages in 2005 through FDA approval in 2015. PeaceHealth adopted the method in 2017, and now he administers the technique, which helps others avoid the unfortunate situation his grandfather couldn’t.
“I wish we’d had this back in 1996 when my grandpa died,” says Dr. MacGregor. “These stories are actually quite common, and I think most people know someone who has been affected in a similar way.”
Atrial Fibrillation (AFib), a form of irregular heartbeat, causes rapid but ineffective beating of the upper chambers of the heart (the atria). There is a pouch called the appendage that is connected to the left atrium. As blood pumps through all the chambers of your heart during each heartbeat, “the place where it moves the slowest is the pouch,” Dr. MacGregor explains. “As blood moves down into the pouch, it moves slower and slower, and it can eventually sludge and clot.” The clot can then travel to the brain and cause a stroke.
“The left atrial appendage is a bit like your appendix; it’s there, but your body doesn’t need it for you to survive,” says Dr. MacGregor.
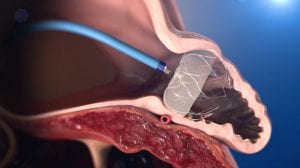
The WATCHMAN procedure stops blood from entering the left atrial appendage, significantly decreasing the chance of blood clots forming. It is designed for certain AFib patients as an alternative to blood thinners.
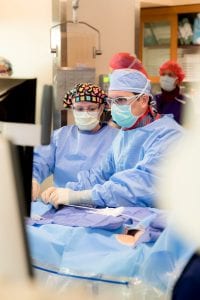
During the procedure, Dr. MacGregor works with a colleague who performs an echocardiogram, or ultrasound, of the heart. This allows him to see into the heart and complete the procedure without opening the patient’s chest cavity. The heart is accessed from a tube, or sheath, that is placed in a large vein in the patient’s groin.
Dr. MacGregor carefully places the WATCHMAN device through the end of the sheath into the mouth of the left atrial appendage to obstruct the blood from flowing into the pouch. It looks like a tiny umbrella that blocks blood from entering the chamber.
Once he is satisfied that the device is sitting right where he wants it to be, he unscrews the WATCHMAN from the sheath and leaves it there. “Your body grows a layer of cells over the device, walling it off,” explains Dr. MacGregor. “After a few months, there’s tissue over it, and it grows into the lining of the left atrium.”
It becomes a part of the patient’s body, essentially blocking the potential for future blood clots in the appendage.
And this amazing procedure is usually completed in only one hour.
“People typically spend one night in the hospital, and we monitor for signs of complications. And then they’re back to see us one week later,” Dr. MacGregor says.
Recovery is relatively painless; patients skip the gym for a week, and then it’s back to living their lives.
Recipients of the WATCHMAN typically take blood thinners for only six months after surgery, and then switch to aspirin. “The real benefit of this procedure lies in the ability to get people off blood thinners afterward,” explains Dr. MacGregor. “Recall what happened to my grandpa; if he’d been able to stop coumadin safely, his story may have had a very different ending.”
Roughly one in three AFib patients will have a stroke during their lifetime. Those who get appropriate treatment (the WATCHMAN being one excellent option for some) reduce those odds substantially.

“Baby boomers are aging, and they’re hitting the stage where the likelihood of developing atrial fibrillation increases,” says Dr. MacGregor. “Right now, there are approximately five million Americans with AFib, and some estimates suggest that number could double by 2030.”
Before the WATCHMAN procedure, the only nonsurgical option was to put patients on blood thinners long term. Now there’s a permanent solution that doesn’t involve heart surgery.
“Right after we started the program here, my uncle called me and said, ‘My cardiologist just talked to me about this thing called the WATCHMAN,’” says Dr. MacGregor. “I said, ‘Uncle Bruce, I’m a firm believer in this technology. If you’re a candidate, I say go for it.’ He now has a WATCHMAN, and he’s doing great.”
For more information on the WATCHMAN, contact the PeaceHealth St. Joseph Medical Center Cardiovascular Center.
Sponsored